|

by Emily Mullin
November 01,
2018
from
Medium Website
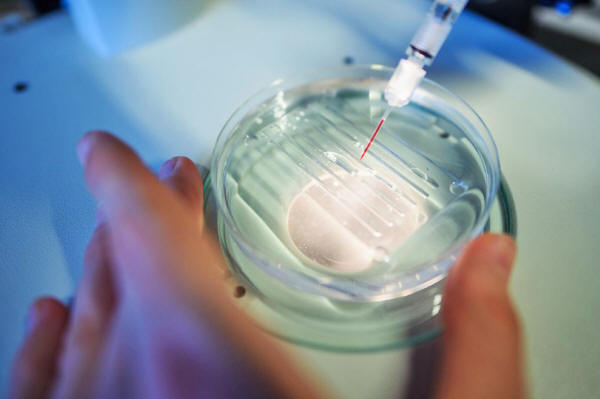
From
turning pigs into organ donors
to changing the
color of flowers,
the future of
gene-editing tech
is wacky and
wonderful...
There are few modern-day scientific innovations with implications as
profound as the
gene-editing technology CRISPR,
which allows scientists to precisely cut and alter the DNA of any
cell.
Scientists' use of CRISPR
has taken off, in part because it's so much easier to use than
earlier iterations of gene editing. Though CRISPR hasn't cured
disease or ended world hunger yet, it's already being used in some
amazing ways.
We've rounded up seven of
the most wild examples.
1. Turning
pigs into organ donors
For decades, scientists have considered the controversial idea that
animals could provide a ready supply of organs to help ease the
organ transplant shortage.
More than 114,000 people
are currently waiting to receive a transplant in the U.S., alone.
Past attempts to implant animal organs into people have failed
because the human body's immune system rejects foreign tissue. (The
first heart transplant ever performed in a human was in 1964, with a
chimpanzee heart. The patient died within two hours.)
Another barrier is the
possibility that infections from animal donors could be transmitted
to human recipients.
Researchers think CRISPR could solve both of these challenges.
One company,
eGenesis, spun out of Harvard
geneticist George Church's lab, is using CRISPR to make pigs
suitable organ donors for humans. Many pig organs, like the heart
and lungs, are similar in size to human ones.
Researchers at eGenesis have used CRISPR to
snip out a family of viruses found
in pig DNA that could be passed to people during transplantation.
These viruses, known as
porcine endogenous retroviruses, or
PERVs, could jump from pigs to
human cells and randomly integrate into the human genome.
The company has produced
dozens of virus-free pigs so far. The company is also using CRISPR
to modify genes involved in the immune system and prevent the human
body from rejecting the organs.
A clinical trial of human
transplants with organs produced in gene-edited pigs is, most
likely, still years away.
"I think people
wanted this to happen because they realized it was the ultimate
medicine."
2. Making new
and improved fruit
You're probably not familiar with groundcherry (physalis),
but Joyce Van Eck hopes the fruit will someday become a
household name.
About the size of a cherry tomato, the groundcherry is sweet with
notes of pineapple and mango. It can grow in the U.S., but it's
currently uncommon because the plants sprawl wildly and are hard to
control.
Eck, an associate professor at Cornell University, and her
collaborator Zachary Lippman at the Cold Spring Harbor
Laboratory, are using CRISPR to make the groundcherry more appealing
to farmers.
"We saw it as a
novelty fruit that, with some improvement, could become a more
specialty food crop in the U.S. and grow more widely," Eck says.
Eck and Lippman first
targeted the groundcherry's self-pruning gene to make the plant more
compact as it grows.
Eck says the change
essentially fast-tracked the plant's domestication and made the
fruit develop earlier. Next, they used CRISPR to tweak the
groundcherry's genetics to make the fruit 25 percent bigger.
They published their
findings (Rapid
Improvement of Domestication Traits in an Orphan Crop by Genome
Editing) in October 2018, in the journal Nature Plants.
Eck thinks CRISPR will be an important tool in domesticating new
crops, increasing the nutritional value of food, and helping to
protect crops from extreme weather and climate change.
"We rely on just a
handful of staple food crops, not just within the U.S. but in
other countries," she says. "I think it's really important to
find other crops in case of crop failure, but also as a way to
diversify diets."
CRISPR is also being
studied as a way to
breed cacao trees to be resistant
to diseases that are increasingly affecting chocolate production.
And
DuPont Pioneer, an agriculture
company, has licensed CRISPR technology to breed a new and improved
variety of waxy corn, which is used to thicken food products.
3. Changing
flowers from violet to white
Japanese scientists are using CRISPR to change the flower color of a
traditional garden plant.
Researchers programmed CRISPR to target a specific gene, known as
DFR-B gene, in the Japanese morning
glory. In the lab, they inserted the CRISPR system into plant
embryos.
The gene-editing tool
successfully disrupted the DFR-B gene, which is responsible for the
color of the plant's stems, leaves, and flowers. By doing so, it
changed the plant's characteristic violet color to white.
The researchers say their work (CRISPR/Cas9-mediated
mutagenesis of the dihydroflavonol-4-reductase-B locus in the
Japanese morning glory Ipomoea -Pharbitis- nil),
published last year, reveals the huge potential of CRISPR to the
study and manipulation of genes in gardening plants.
4. Modifying
human embryos for healthier babies
Last year, a scientist in Oregon made headlines when
he reported that his team used
CRISPR to snip out a heart disease-causing genetic error in dozens
of human embryos.
It was the first time
CRISPR had been used in the U.S. to modify human embryos.
Shoukhrat Mitalipov, who directs the
Center for Embryonic Cell and Gene Therapy
at Oregon Health and Science University, zeroed in on a mutation in
a gene called MYBPC3 which is responsible for an inherited heart
condition called hypertrophic cardiomyopathy.
The condition occurs in
about 1 in 500 people and can cause heart failure and sudden death.
"Every generation on
would carry this repair because we've removed the
disease-causing gene variant from that family's lineage,"
Mitalipov said in a university statement.
Editing cells in embryos
is known as
germline editing, and is
controversial because the genetic changes that result can be passed
on to subsequent generations.
That's different than
somatic genome editing, which only affects the treated
individual.
Japan may soon move forward with similar research. The country has
issued draft guidelines allowing human embryos to be modified with
CRISPR and other genome-editing technologies.
If adopted,
"the guidelines would
restrict the manipulation of human embryos for reproduction,
although this would not be legally binding," according to an
October 2018
report in the journal Nature.
But science is far from
using CRISPR to make designer babies - at least in the U.S.
That's because a
congressional rider forbids the U.S. Food and Drug Administration
(FDA)
from even considering any human trials that would involve modifying
human embryos.
5. Halting
muscular dystrophy in dogs
In dogs with muscular dystrophy, a CRISPR gene-editing treatment
appeared to fix the genetic mutation responsible for disease.
The findings (Gene
Editing restores Dystrophin Expression in a canine model of Duchenne
Muscular Dystrophy), reported in August 2018, represent a
major step forward in developing a treatment for
Duchenne muscular dystrophy, a
devastating and life-shortening illness most common among young
boys.
It's a genetic disease
occurring in about 1 in 3,500 boys born, worldwide.
Duchenne is caused by a mutation in the DMD gene, which makes
dystrophin, an essential protein
found in muscle cells. The mutation means the gene can't make
functioning dystrophin, and without it, muscles are weak and don't
work properly.
Muscle loss in
Duchenne is typically fatal, and men with the disorder usually
only reach their early thirties.
In an effort to stop the disease in its tracks, researchers at the
University of Texas Southwestern injected CRISPR into one-month-old
beagles. Gene editing was able to restore dystrophin in muscle and
heart tissue in the dogs by up to 92 percent.
Scientists have estimated
that a 15 percent threshold would be needed to significantly help
humans.
"It is really
impressive how well this works," says Elizabeth McNally,
director of the Center for Genetic Medicine at Northwestern
University, who studies the genetics of muscular dystrophy.
Elizabeth McNally
wasn't involved in the research, but serves on the board of
Exonics, the company that funded
the study.
"You see this change
where a small amount of DNA being corrected can result in a big
protein change."
McNally says she wouldn't
be surprised if the approach moved to human trials in just a few
years.
"I think in many
ways, Duchenne is really the poster child for doing
this," she says of gene editing.
6. Creating
new treatments for cancer and blood disorders
Injecting CRISPR directly into the body is risky, so for now,
investigators are using CRISPR to edit human cells outside the body
and then infusing them back into patients.
The approach is being
used in early clinical trials in the U.S., Europe, and China.
In the U.S., a trial sponsored by the University of Pennsylvania and
a company called
Tmunity is recruiting up to 18
people with multiple myeloma, sarcoma, and melanoma who haven't
responded to traditional drugs, or have seen their cancer come back.
Investigators will
extract human immune cells from the men and women and use CRISPR to
genetically alter them to attack cancer cells. The edited cells will
then be infused back into the patients.
Another company,
CRISPR Therapeutics, is planning to
use CRISPR to treat people with beta thalassemia and sickle cell
disease, two related blood disorders that are caused by mutations in
the same gene.
These mutations affect a
person's ability to make hemoglobin, a vital protein in red blood
cells that carries oxygen throughout the body. In a statement
provided to Medium, the company said it started enrolling people
with beta thalassemia into a clinical trial in Germany.
Meanwhile, in the U.S.,
CRISPR Therapeutics and Vertex Pharmaceuticals are planning to
launch a trial for sickle cell by the end of 2018.
Both trials will extract bone marrow stem cells from people in the
trial, edit the cells with CRISPR in the lab, and transfer them back
into the patients. They hope that the process helps patients produce
a type of hemoglobin.
Researchers in China began their first round of similar experiments
in people last year, but have yet to report any data from the
11 ongoing trials registered on
clinicaltrials.gov.
Eric Kmiec, director of the Gene Editing Institute at
Christiana Care Health System in Delaware, says he's not surprised
that CRISPR has moved this quickly for very serious diseases.
"I think people
wanted this to happen because they realized it was the ultimate
medicine," he says. "Considering the desperation and lack of
other treatments for some diseases, it's encouraging."
7. Eliminating
mosquitoes
Mosquito-borne diseases, especially malaria, are a deadly scourge.
Globally, malaria kills
more than 400,000 people every year. To cut down on the spread, some
scientists propose using a controversial technology called a
gene drive.
A gene drive is a genetic engineering tool designed to spread
certain genes throughout a species. Though it's not a new idea, gene
drives are closer to reality now thanks to CRISPR.
In a paper (A
CRISPR–Cas9 Gene Drive targeting Doublesex causes complete
Population Suppression in caged Anopheles gambiae Mosquitoes)
published in September 2018, researchers at Imperial College London
showed that a gene drive made with CRISPR could suppress a
population of Anopheles gambiae - the type of mosquito that
transmits malaria in Sub-Saharan Africa.
Investigators used CRISPR to target alter a so-called doublesex
gene, which is responsible for female development.
When female mosquitoes
inherited two copies of this modified gene, they couldn't bite or
lay eggs. Researchers tested the self-destructive mosquitoes in
cages and found that, after eight generations, no normal females we
left to reproduce and the population died out.
Genes drives haven't been released outside of laboratories
yet.
There's the possibility
that genetic alterations designed to crash populations could mutate
and pass on an advantageous trait. But this study showed that the
gene drive transmitted the genetic modification nearly 100 percent
of the time, avoiding resistance.
Leaders of the African Union earlier this year endorsed
gene drive research in an effort to
fight malaria in their countries, but it could still be years before
the technology is tested in the wild.
|