|
January 23, 2011 from NewsWeek Website
If you follow the news about health research, you risk whiplash.
First garlic lowers bad cholesterol, then - after more study - it doesn’t. Hormone replacement reduces the risk of heart disease in postmenopausal women, until a huge study finds that it doesn’t (and that it raises the risk of breast cancer to boot). Eating a big breakfast cuts your total daily calories, or not - as a study released last week finds.
Yet even if biomedical research can be a
fickle guide, we rely on it.
But what if wrong answers aren’t the exception but the rule?
More and more scholars who scrutinize health research are now making that claim. It isn’t just an individual study here and there that’s flawed, they charge. Instead, the very framework of medical investigation may be off-kilter, leading time and again to findings that are at best unproved and at worst dangerously wrong.
The result is a system that leads patients and physicians astray - spurring often costly regimens that won’t help and may even harm you. It’s a disturbing view, with huge implications for doctors, policymakers, and health-conscious consumers.
And one of its foremost advocates, Dr. John P.A. Ioannidis, has just ascended to a new, prominent platform after years of crusading against the baseless health and medical claims.
As the new chief of Stanford University’s Prevention Research Center, Ioannidis is cementing his role as one of medicine’s top myth-busters.
This is Ioannidis’s moment.
As medical costs hamper the economy and impede deficit-reduction efforts, policymakers and businesses are desperate to cut them without sacrificing sick people. One no-brainer solution is to use and pay for only treatments that work.
But if Ioannidis is right, most
biomedical studies are wrong.
Cost of statins:
In November a panel of the Institute of Medicine concluded that having a blood test for vitamin D is pointless:
Cost of vitamin D:
Ioannidis, 45, didn’t set out to slay medical myths.
A child prodigy (he was calculating decimals at age 3 and wrote a book of poetry at 8), he graduated first in his class from the University of Athens Medical School, did a residency at Harvard, oversaw AIDS clinical trials at the National Institutes of Health in the mid-1990s, and chaired the department of epidemiology at Greece’s University of Ioannina School of Medicine.
But at NIH Ioannidis had an epiphany.
“Positive” drug trials, which find that a treatment is effective, and “negative” trials, in which a drug fails, take the same amount of time to conduct.
With billions of dollars on the line, companies are loath to declare a new drug ineffective. As a result of the lag in publishing negative studies, patients receive a treatment that is actually ineffective.
That made Ioannidis wonder, how many biomedical studies are wrong? His answer, in a 2005 paper: “the majority.”
From clinical trials of new drugs to cutting-edge genetics, biomedical research is riddled with incorrect findings, he argued. Ioannidis deployed an abstruse mathematical argument to prove this, which some critics have questioned.
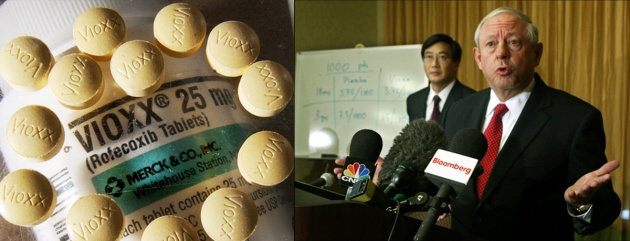
Medical Breakthroughs and Breakdown Joe Raedle / Getty Images
Vioxx: Once a popular treatment for arthritis and hailed for its ability to decrease pain and increase mobility, Vioxx saw its fortunes decline precipitously. More than five years after it was approved by the FDA, manufacturer Merck withdrew the drug from the market
when it emerged
that long-term patients had an increased risk of heart attack and
stroke. a press conference announcing the company’s withdrawal of the drug.
Thalidomide: Thalidomide was not only an effective sedative, it was particularly useful in treating morning sickness, and so it was popular with pregnant women for several years beginning in the late 1950s. But the drug turned out to have horrific side effects: children of women who’d taken it were born with deformed limbs, and thalidomide was withdrawn in 1961.
However, more
recent research has shown than it can be effective in combating some
bone cancers. because her mother took Thalidomide tries out new artificial limbs.
Fen-Phen: A combination of fenfluramine and phentermine, fen-phen was prescribed widely - some 6 million patients took the drug—in the ’90s as a weight-loss medication. Initial reports - both through word of mouth and heavy marketing - credited it for rapid weight loss with minimal side effects (at left, a Nashville, Tenn., clinic advertises fen-phen). But the drug was recalled in 1997 when research revealed that use, even over a short period of time, could cause serious and even fatal damage to the heart valves and the lungs.
Even a cursory glance at medical journals shows that once heralded studies keep falling by the wayside.
Two 1993 studies concluded that vitamin E prevents cardiovascular disease; that claim was overturned by more rigorous experiments, in 1996 and 2000. A 1996 study concluding that estrogen therapy reduces older women’s risk of Alzheimer’s was overturned in 2004.
Numerous studies concluding that popular
antidepressants work by altering brain chemistry have now been
contradicted (the drugs help with mild and moderate depression, when
they work at all, through a placebo effect), as has research
claiming that early cancer detection (through, say, PSA tests)
invariably saves lives. The list goes on...
Ioannidis’s first targets were shoddy statistics used in early genome studies.
Scientists would test one or a few genes at a time for links to virtually every disease they could think of. That just about ensured they would get “hits” by chance alone.
When he began marching through the genetics literature, it was like Sherman laying waste to Georgia:
Statistical flukes also plague epidemiology, in which researchers look for links between health and the environment, including how people behave and what they eat.
A study might ask whether coffee raises the risk of joint pain, or headaches, or gallbladder disease, or hundreds of other ills.
Drug companies make a mint on such dicey statistics.
By testing an approved drug for other uses, they get hits by chance,
Even when a claim is disproved, it hangs around like a deadbeat renter you can’t evict.
Years after the claim that vitamin E prevents heart disease had been overturned, half the scientific papers mentioning it cast it as true, Ioannidis found in 2007. The situation isn’t hopeless. Geneticists have mostly mended their ways, tightening statistical criteria, but other fields still need to clean house, Ioannidis says.
Surgical practices, for instance, have not been tested to nearly the extent that medications have.
That would also save billions of dollars.
George Lundberg, former editor of
The Journal of the American Medical Association (JAMA), estimates that
strictly applying criteria like Ioannidis pushes would save $700
billion to $1 trillion a year in U.S. health-care spending.
Smoking kills, being morbidly obese or severely underweight makes you more likely to die before your time, processed meat raises the risk of some cancers, and controlling blood pressure reduces the risk of stroke.
The upshot for consumers:
|