|
by Dave Mihalovic December 12, 2016
from
PreventDisease Website
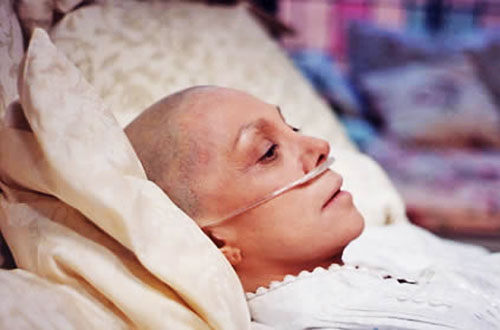
Heart damage caused by chemotherapy is worse in cancer patients with metabolic diseases, according to a study presented EuroEcho-Imaging 2016. The overall contribution of cytotoxic chemotherapy to 5-year survival in adults is well below 3 percent.
Oncologists are now being advised that
this toxic treatment has dire
consequences for those with metabolic diseases such as diabetes and
insulin resistance.
Cardiac damage can occur even with lower doses of drugs if the person has had previous radiation and specific types of drug therapy.
She continued:
Hospital Garcia de Orta has a surveillance program, run by Cardiology, Oncology and Haematology, to monitor cancer patients who receive anthracycline-based chemotherapy.
Clinical and echocardiographic evaluation is conducted before, during and after chemotherapy, regardless of whether or not the patient has symptoms. The aim is to detect cardiotoxicity early so that heart failure can be prevented.
In her research Dr Ana Catarina Gomes investigates factors that could affect the likelihood of patients having heart damage after treatment with anthracyclines. The current study assessed the impact of cardiovascular risk factors and type of cancer on the development of cardiotoxicity to help identify patients at greater risk.
The study included all 83 patients in the surveillance program, of whom 54 had breast cancer, 20 had lymphoma, and nine had gastric cancer.
For each patient, data was collected on demographics, cardiovascular risk factors (hypertension, diabetes mellitus, dyslipidaemia, smoking), previous cardiovascular and non-cardiovascular diseases, and type and cumulative dose of anthracyclines.
Echocardiographic evaluation included
heart chamber dimensions, systolic and diastolic function, ejection
fraction and global longitudinal strain. Measurements were performed
before chemotherapy was started, during treatment, and after the end
of chemotherapy.
A total of 39 patients were treated with doxorubicin and 44 received epirubicin. Cumulative doses were within recommended ranges. Patients were 52 years old on average (range 39 to 65 years) and 78% were female.
Some,
Overall, global longitudinal strain and left ventricular ejection fraction progressively decreased and were significantly lower after chemotherapy compared to baseline.
Patients with hypertension showed a trend toward greater reductions in ejection fraction. Patients with diabetes had a significantly greater decrease in global longitudinal strain during treatment, despite having baseline levels similar to non-diabetics.
Dr Gomes said:
|