|

by Ryan Browne
August 17,
2018
from
CNBC Website
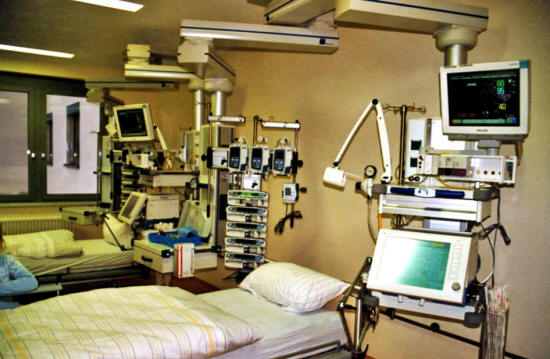
Wikimedia Commons
Technocrat A.I. scientists who are not trained
physicians will ultimately dominate doctors for
patient diagnosis and treatment.
They say that doctors will simply have to
adapt...
Meanwhile, doctors are pushing back to maintain
their role as the primary care giver.
Source
Tech firms say
A.I. can transform health care as we know it - Doctors think they
should slow down
As an industry reliant on
patient records and beset by outdated technology, health care is
widely thought to be a prime target for an artificial intelligence
revolution.
Many believe the technology will provide a host of benefits to
clinical practitioners, speeding up the overall experience and
diagnosing illnesses early on to identify potential treatment.
Just two days ago,
DeepMind, an A.I. (artificial
intelligence) firm owned by Google, said it had lent its
technology to London's Moorfields Eye Hospital for groundbreaking
research into detecting eye diseases.
It was used to scan and
identify more than 50 ophthalmological conditions. DeepMind's
machine-learning technology made correct diagnoses 94 percent of the
time, Moorfields said.
The development indicated that A.I. can analyze health problems with
as much accuracy as a doctor. But some doctors worry that those in
the tech world think A.I. can not only help clinicians, but even do
a better job.
Take
Babylon Health for instance, which in June said its A.I.
chatbot was able to diagnose medical conditions as accurately as a
doctor.
The firm's chatbot scored
a higher-than-average test score on the official exam set for
physicians by the Royal College of General Practitioners (RCGP), an
industry body representing GPs - doctors that treat a wide range of
common illnesses.
Babylon's chatbot passed 82 percent of the test's questions, versus
the average mark for human doctors of 72 percent.
But the RCGP quickly disputed the claim that A.I. could diagnose
illnesses with the same effectiveness of a human medical
practitioner.
"No app or algorithm
can do what a GP does," Helen Stokes-Lampard, a professor and
chair of the RCGP, told CNBC earlier this week.
"Every day we deliver
care to more than a million people across the U.K., taking into
account the physical, psychological and social factors that may
be impacting on each person's health."
Helen Stokes-Lampard
continued:
"We consider the
different health conditions a patient is living with, their
family history, any medications they might be taking, and a
myriad of other considerations when formulating a treatment
plan."
Babylon at the time
denied it had claimed an A.I. could do the job of a GP, saying that
it supported a model where A.I. is complementary to medical
practice.
'The role of
the doctor will have to adapt'
Nevertheless, the spat highlighted a serious question that may one
day need to be addressed by those in the health industry:
How should health
professionals respond to the rapid growth in new, data-driven
technologies like A.I.?
"Over the next
decade or two, A.I. will certainly play a big role in
supporting doctors make decisions," Dan Vahdat, chief
executive of health tech start-up Medopad, told CNBC via
email.
"The role of the doctor will have to adapt in learning how
to use A.I. to complement their clinical judgments. This
will take time, but it's inevitable."
Medopad specializes in
connecting health-care providers, doctors and patients to monitor a
patient's health data and see how their care can be improved.
In the U.K., the National Health Service, the country's universal
health care system, has come under strain both in terms of funding
and resources.
The promise of A.I. to
reduce the financial burden on medical services by cutting out some
disposable roles and functions could be music to the ears of
government and health authorities.
Dan Vahdat said that one area in which A.I. could be hugely
beneficial in improving efficiency and cutting costs was
cardiological care.
"If we collect data
in real time and combine it with their historical data as well
as data from millions of similar patients, an intelligent system
could predict a heart attack with a high rate of precision," he
said.
"This will allow us to save countless lives and save health care
systems around the world huge spend."
But some experts fear the
fast-paced nature of the still nascent A.I. industry could come at
the risk of patient safety.
"We are concerned
that in the rush to roll out A.I. and push the boundaries of
technology, there is a risk that important checks and balances
that have been established to keep patients safe might be seen
as an afterthought, or be bypassed entirely," Stokes-Lampard
said.
Last month, a report by
online
health publication Stat said that IBM's Watson supercomputer
had made multiple "unsafe and incorrect" cancer treatment
recommendations, citing internal company documents.
According to Stat, the
program had only been trained to deal with a small number of cases
and hypothetical scenarios instead of actual patient data.
IBM subsequently told
CNBC that it has,
"learned and improved
Watson Health based on continuous feedback from clients, new
scientific evidence and new cancers and treatment alternatives."
Stokes-Lampard said that
regulators should keep pace with the rapid advances in technology to
avoid harm to patients.
She said:
"In an ever-changing
'tech space,' it is imperative that regulation keeps up with all
technological developments, and that it is appropriately
enforced, so that patients are kept safe, however they choose to
access care."
But many tech companies -
big and small - are mostly averse to new regulation, arguing it
could restrain innovation.
"There are a lot of
regulations to protect patients already," Medopad's Vahdat said.
"It isn't about
adding more regulation - it is about adapting and applying
existing regulations to better deal with current realities."
He added:
"Patients as a cohort
are often vulnerable and we feel responsible to not create hope
that is not qualified. We feel strongly that unless our
technology is clinically validated it shouldn't be marketed.
Like doctors, health
care start-ups should seek to fully understand the ethical
implications of creating expectations with patients."
Data
Another concern is data.
For a medical A.I. app,
myriads of patient data are required to optimize analysis of a
patient's health status. That's why firms like Medopad and DeepMind
have partnered with hospitals, gaining access to libraries of
patient information.
But the need for that data has heightened concerns over the privacy
of patients, who would more than likely prefer sensitive records
about their health problems not be inappropriately shared or exposed
through a cyberattack.
Last year, British privacy watchdog the Information
Commissioner's Office (ICO) rapped a hospital working with
DeepMind over its use of patient data.
The Royal Free Hospital
in London had struck a deal with Google's A.I. firm allowing the
company to gain access to the data of 1.6 million patients, but did
not do enough to inform them about how that information would be
used.
"When it comes to
data, the more access to data you can have the better your A.I.
can become," Poppy Gustafsson, chief executive of A.I. and
cybersecurity firm Darktrace, told CNBC.
"But obviously your
data needs to be protected, so where some are trying to develop
systems whereby they are getting a lot of data to try and gather
those learnings, they also need to think about how they are
going to keep that data secure."
Health care is an
important battleground for some of biggest tech companies in the
U.S.,
...are all developing
cloud and A.I. technology aimed at improving the health system.
The RCGP's Stokes-Lampard said that tech platforms ought to be
conscious of their responsibility to protect patients.
"The RCGP is keen to
the see the NHS embrace new technology, and we believe that it
has the potential to transform many aspects of the NHS, but it
must be implemented in a safe and equitable way that doesn't
benefit some patients at the expense of others, and is not to
the detriment of general practice as a whole," she said.
|